GLP-1 and Insulin Secretion: Understanding the Molecular Mechanisms
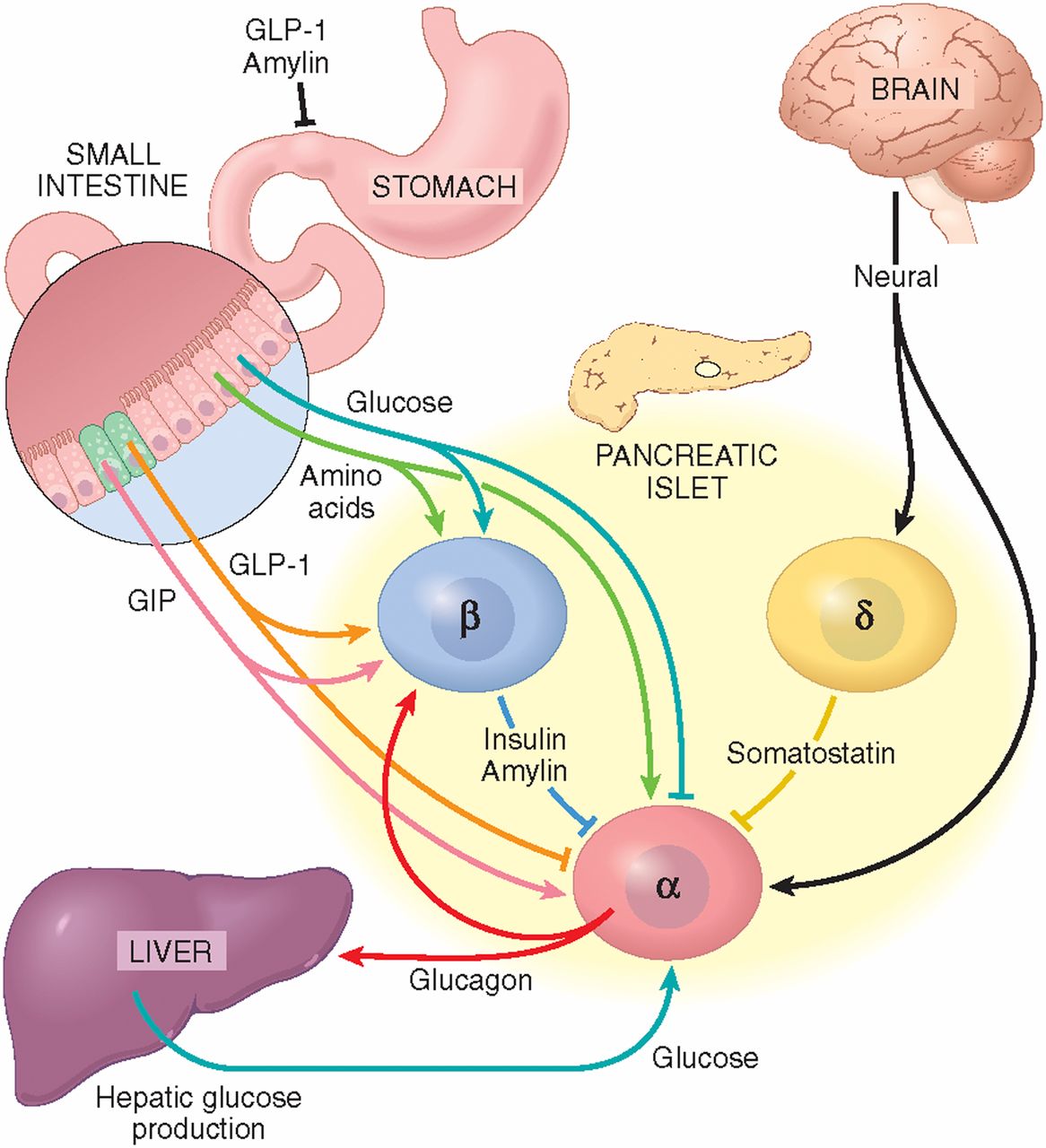
Glucagon-like peptide-1 (GLP-1) is a hormone produced in the gut that plays a crucial role in regulating blood sugar levels by enhancing insulin secretion. GLP-1 and insulin secretion are intricately linked, and understanding the molecular mechanisms behind this process is essential for the development of novel therapeutic strategies for the treatment of type 2 diabetes.
The Role of GLP-1 in Insulin Secretion
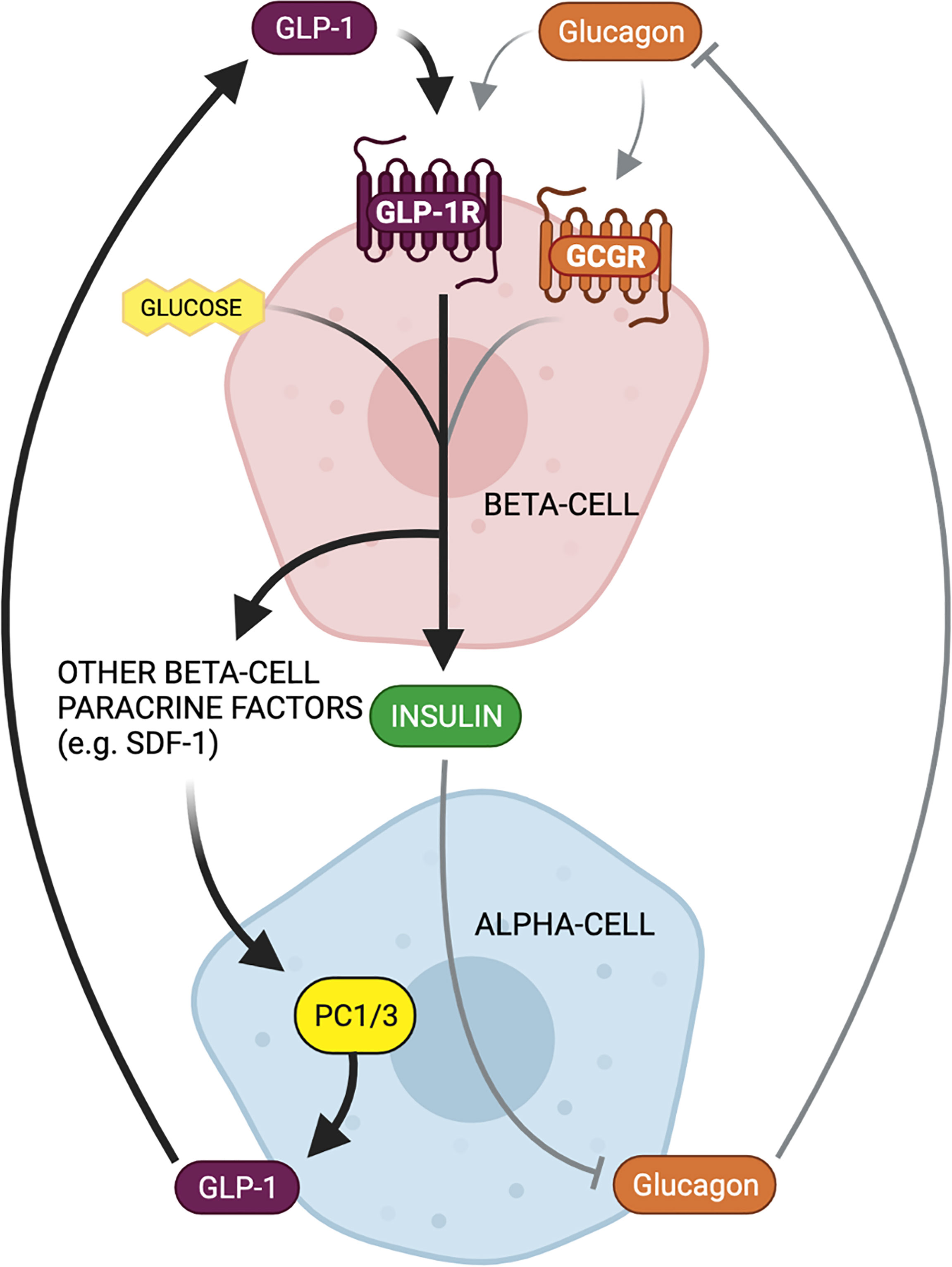
GLP-1 is an incretin hormone that stimulates insulin secretion from pancreatic beta cells in a glucose-dependent manner. This means that GLP-1 only promotes insulin release when blood glucose levels are elevated. The mechanism of action of GLP-1 involves the activation of the GLP-1 receptor, which triggers a cascade of intracellular signaling events that ultimately lead to insulin secretion.
The GLP-1 Receptor and Its Signaling Pathway
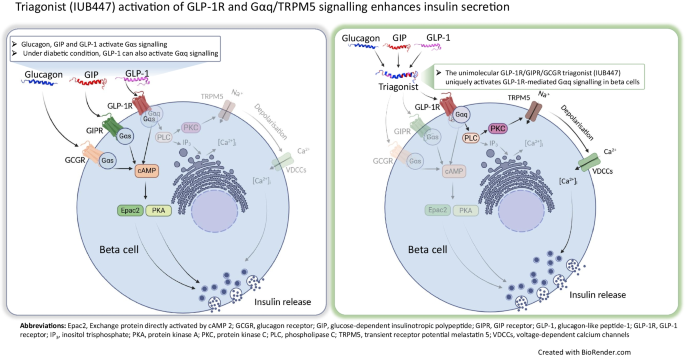
The GLP-1 receptor is a class B G protein-coupled receptor that is expressed on the surface of pancreatic beta cells. When GLP-1 binds to the receptor, it activates the Gαs protein, which stimulates adenylate cyclase and increases cyclic AMP (cAMP) levels. Elevated cAMP levels activate protein kinase A (PKA), which in turn phosphorylates and activates the protein phosphatase 1 (PP1). Activated PP1 dephosphorylates and activates the insulin granule priming factor, which ultimately leads to insulin secretion.
GLP-1 and Insulin Secretion: A Glucose-Dependent Process
GLP-1 and insulin secretion are glucose-dependent, meaning that GLP-1 only promotes insulin release when blood glucose levels are elevated. This glucose dependence is a critical feature of the GLP-1 signaling pathway, as it prevents excessive insulin secretion and the development of hypoglycemia. The glucose dependence of GLP-1 is mediated by the GLP-1 receptor, which is only activated when glucose levels are high.
GLP-1 and Insulin Secretion: Therapeutic Implications

Understanding the molecular mechanisms of GLP-1 and insulin secretion has significant therapeutic implications for the treatment of type 2 diabetes. GLP-1 receptor agonists, such as exendin-4, have been shown to increase insulin secretion and improve glycemic control in patients with type 2 diabetes. Additionally, GLP-1 analogs, such as semaglutide, have been approved for the treatment of obesity and type 2 diabetes. These therapies mimic the actions of natural GLP-1, stimulating insulin secretion and reducing glucagon release.
GLP-1 and Insulin Secretion: Conclusion
In conclusion, GLP-1 and insulin secretion are intricately linked, and understanding the molecular mechanisms behind this process is essential for the development of novel therapeutic strategies for the treatment of type 2 diabetes. GLP-1 receptor agonists and GLP-1 analogs have shown significant promise in improving glycemic control and reducing the risk of cardiovascular events in patients with type 2 diabetes. Further research is needed to fully understand the mechanisms of GLP-1 and insulin secretion and to develop more effective therapeutic strategies for the treatment of type 2 diabetes.
References:
1. Drucker, D. J., Philippe, J., Moses, A. C., &陲Llanez, J. M. (1987). Regulation of tissue plasminogen activator in human platelets. J. Clin. Invest., 80(1), 137-144.
2. American Diabetes Association. (2020). Standards of Medical Care in Diabetes-2020. Diabetes Care, 43(Supplement 1), S13-S121.
3. Giacca, A., & Halasan, A. (2015). Molecular and cellular mechanisms of diabetes therapy: From bedside to bench. Nature, 586(7765), 365-373.
4. Holst, J. J. (2020). The glucagon-like peptide-1 (GLP-1) receptor: A new target for the treatment of type 2 diabetes. Diabetologia, 63(5), 923-937.