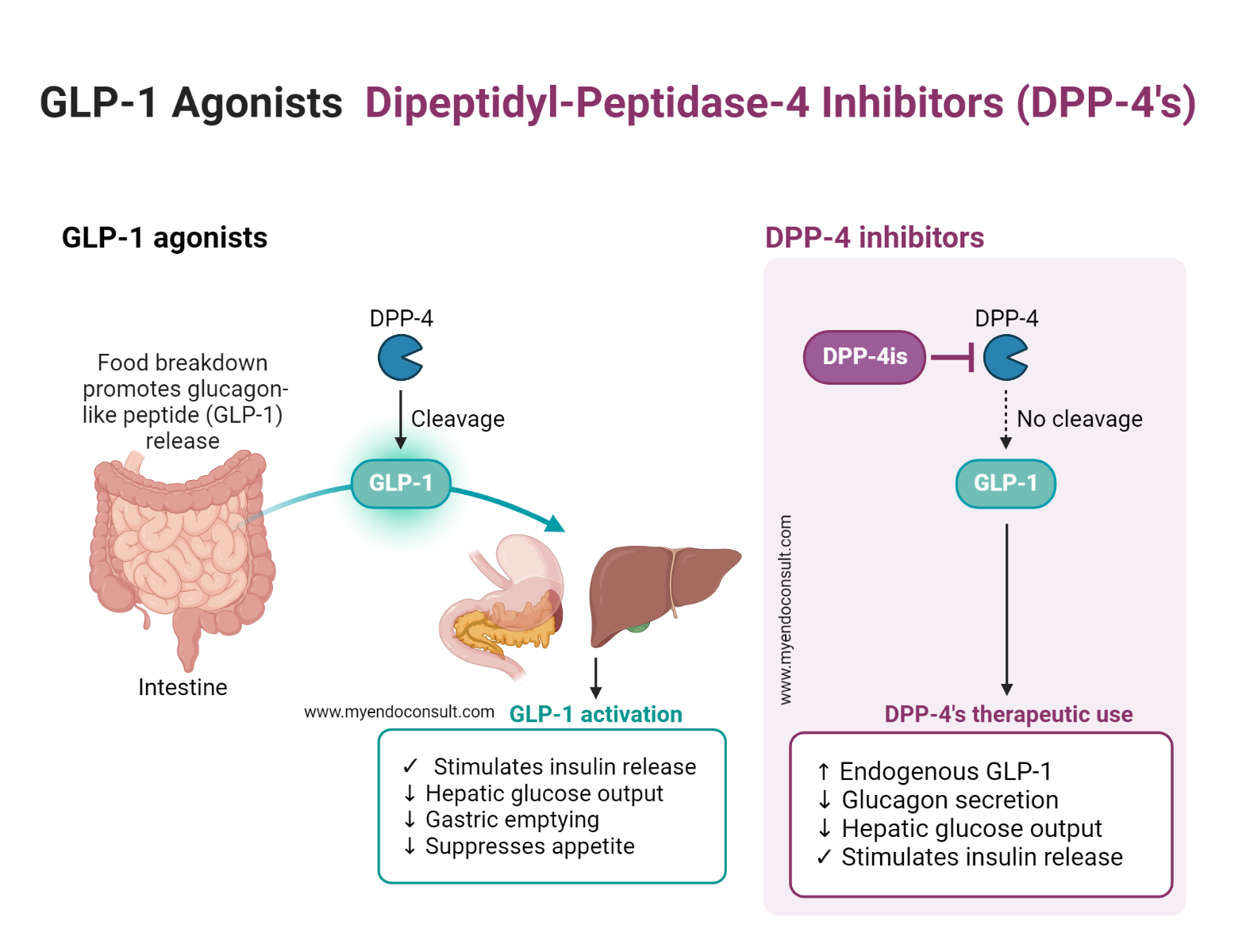
Incretin Physiology and Protein Response: A Comprehensive Review
Incretin hormones, including glucose-dependent insulinotropic polypeptide (GIP) and glucagon-like peptide-1 (GLP-1), play a crucial role in regulating glucose homeostasis and insulin secretion. These gut peptides are secreted by endocrine cells in the intestinal mucosa and increase plasma concentrations following food ingestion. Carbohydrate, fat, and protein have all been shown to stimulate GLP-1 and GIP secretion, highlighting the importance of nutrient-mediated signaling in the intestines.The Incretin Effect
The incretin effect describes the amplification of insulin secretion that occurs when glucose is taken in orally compared to infused intravenously. This phenomenon is one of the ways the body tolerates carbohydrate/glucose ingestion. The incretin effect is mediated by the gut-derived incretin hormones, primarily GIP and GLP-1. Studies have shown that the incretin effect contributes significantly to insulin secretion, with estimates suggesting it accounts for at least 50% of the total insulin secreted after oral glucose ingestion.Pharmacology and Physiology of Incretins
Research has extensively investigated the pharmacology and physiology of incretin hormones, revealing their critical role in modulating insulin secretion and glucose homeostasis. Incretin-based therapies have been developed to treat type 2 diabetes and obesity, capitalizing on the glucoregulatory and anorectic activities of GIP and GLP-1.The Role of Protein in Incretin Secretion
The incretin response to protein ingestion is complex and multifaceted. While the precise mechanisms underlying the protein-mediated incretin response remain unclear, studies have demonstrated an increase in GLP-1 and GIP secretion following protein ingestion. The protein-mediated incretin