Understanding the Role of GLP-1 in Improving Insulin Sensitivity
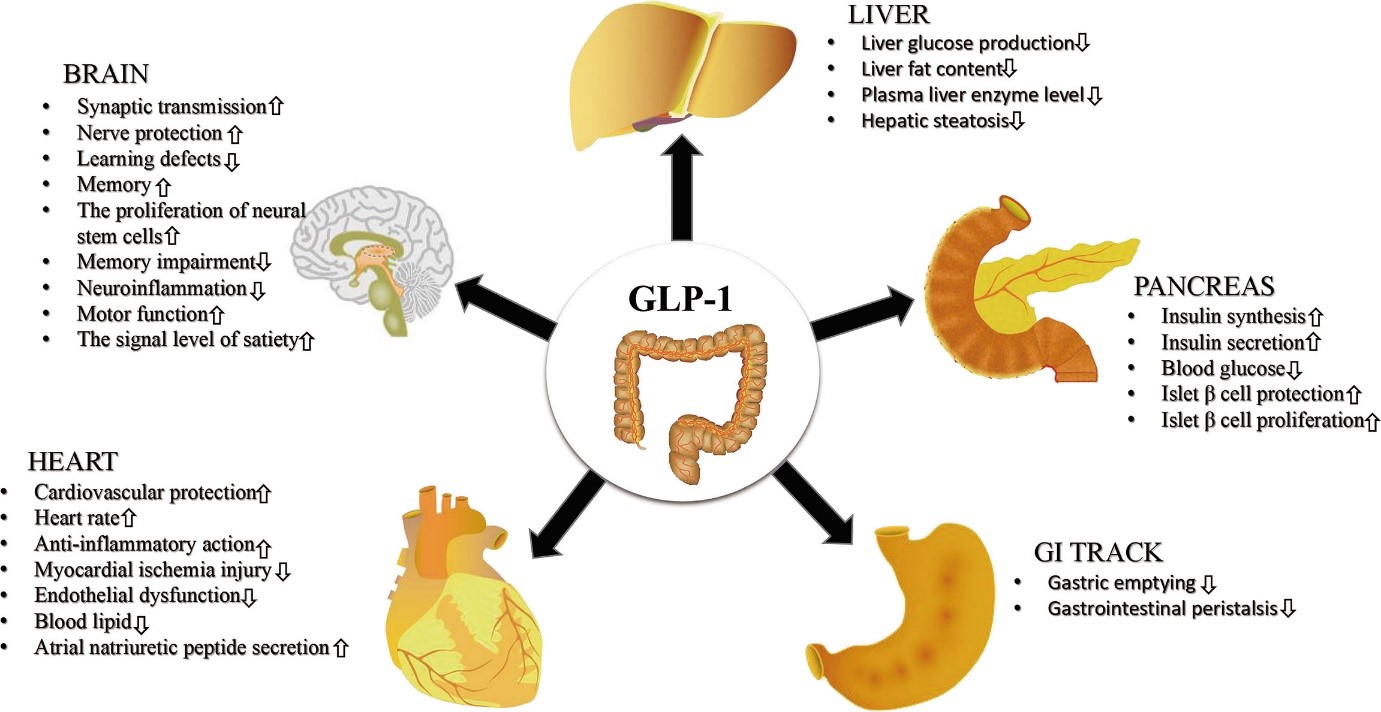
Glucagon-like peptide-1 (GLP-1) is a hormone that plays a critical role in regulating blood sugar levels, appetite, and metabolic balance. GLP-1 receptor agonists, a class of medications, mimic this hormone to improve glycemic control and facilitate weight loss. In this article, we will delve into the role of GLP-1 in improving insulin sensitivity and its implications for managing type 2 diabetes and associated metabolic disorders.
GLP-1 and Insulin Sensitivity
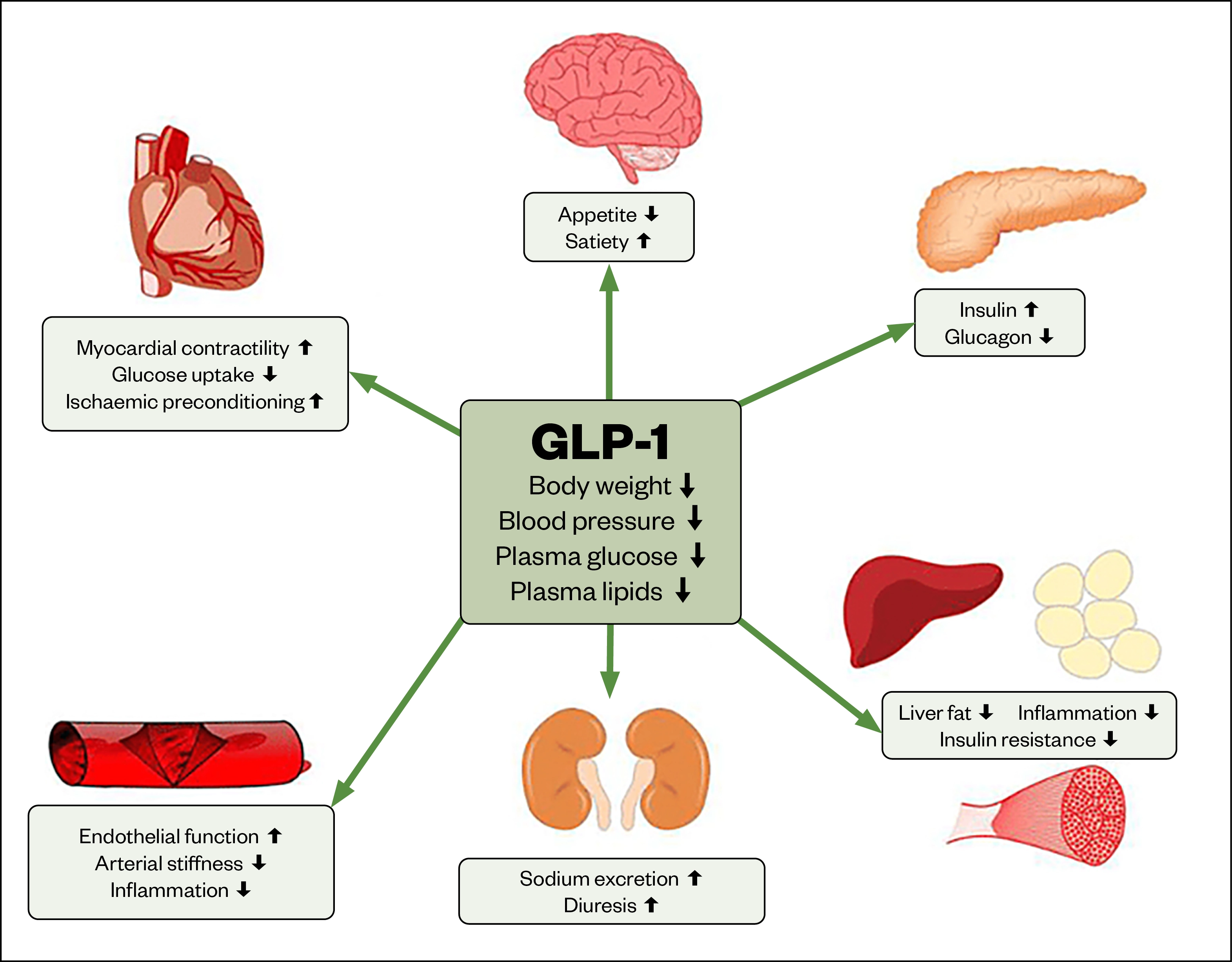
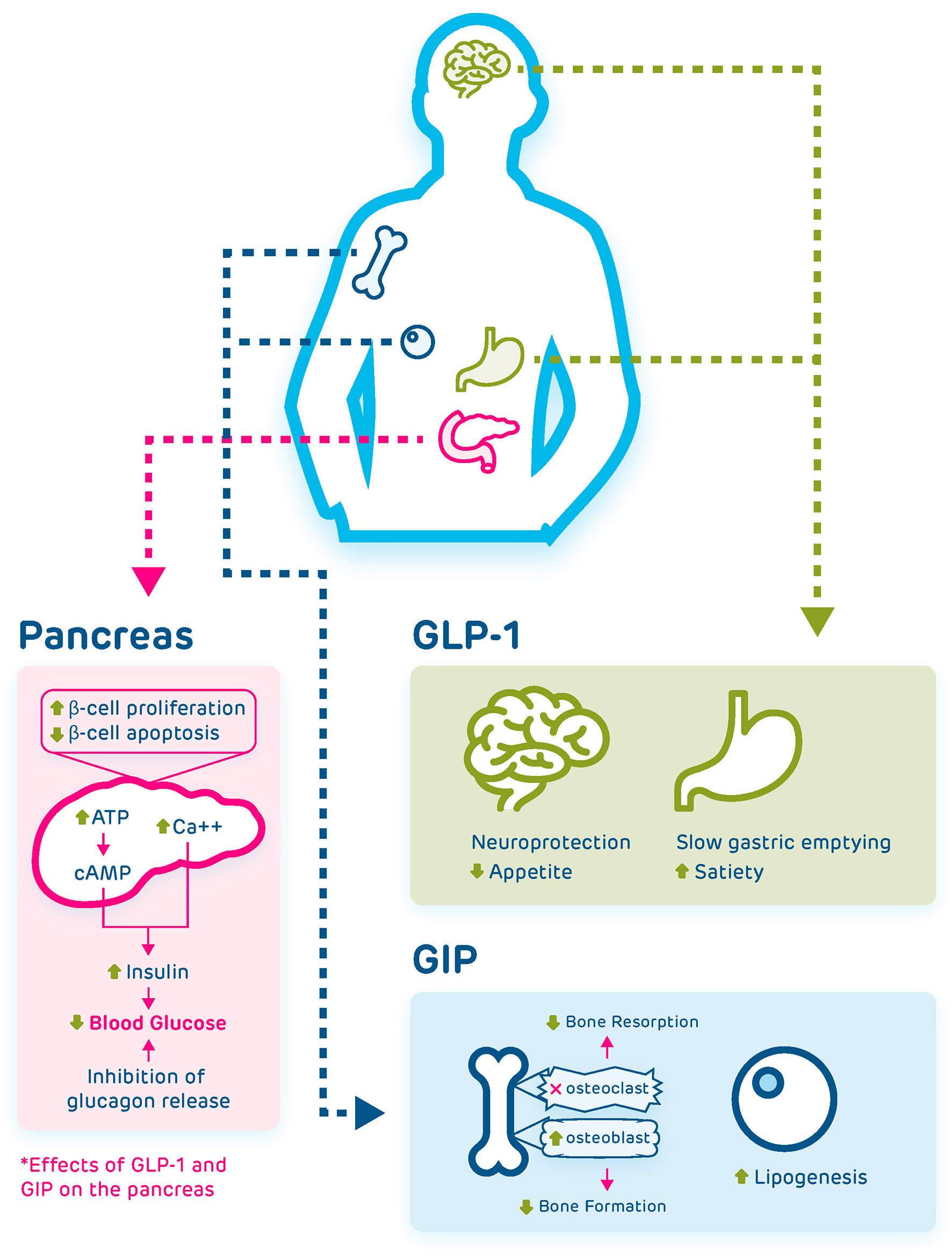
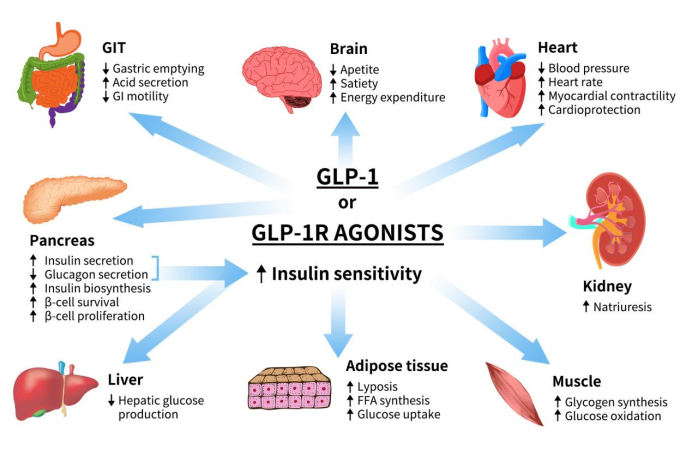
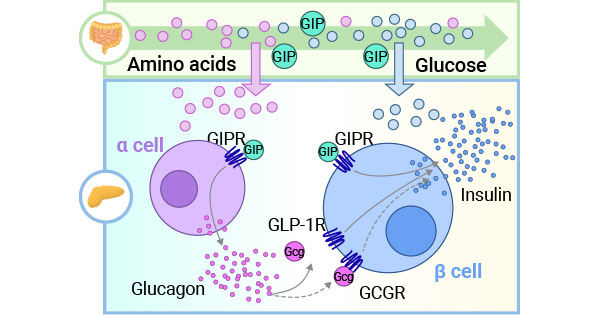
GLP-1 enhances glucose-dependent insulin secretion and reduces glucagon output from pancreatic alpha cells. This sophisticated feedback loop maintains stable blood sugar levels by coordinating insulin and glucagon release in response to food intake. Research has shown that GLP-1 treatments reduce markers of insulin resistance, much of which stems from moderate, consistent weight loss that improves metabolic function.
GLP-1's Role in Improving Peripheral Insulin Sensitivity
While early studies suggested that GLP-1 might not directly improve peripheral insulin sensitivity, more recent evidence demonstrates that GLP-1 receptor agonists do improve insulin resistance through multiple mechanisms. These mechanisms include enhancing insulin signaling pathways and increasing glucose effectiveness, making GLP-1 a crucial player in managing insulin resistance and alleviating symptoms associated with type 2 diabetes.
Key Mechanisms of GLP-1 in Improving Insulin Sensitivity
- Enhancing glucose uptake in tissues
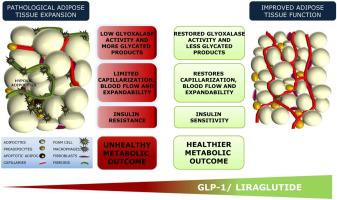
- Reducing inflammation
- Improving blood vessel function
- Supporting weight loss and metabolic efficiency
Importance of Physical Activity in Combining with GLP-1 Therapy
Physical activity complements GLP-1 therapy by improving insulin sensitivity, increasing calorie expenditure, and promoting muscle growth. By pairing physical activity with GLP-1 medications, individuals can enhance their overall metabolic health and mitigate the risk of developing insulin-related disorders.
Personalized Nutrition Strategies and GLP-1 Secretion
Customized nutrition strategies, such as those that support natural GLP-1 secretion and stable blood sugar, can be an effective adjunct to GLP-1 therapy. Additionally, gut healing protocols can improve microbiome balance and reduce inflammation, further amplifying the therapeutic benefits of GLP-1.
GLP-1's Role in Treating Polycystic Ovary Syndrome (PCOS)
GLP-1 medications can improve fertility in women with PCOS through weight loss and insulin sensitivity. Weight loss from GLP-1 therapy may restore ovulation in women with obesity-related fertility issues. However, discontinuing GLP-1 drugs before planned pregnancy is recommended due to limited safety data, highlighting the need for monitoring and personalized care.
Research on GLP-1 and its effects on fertility in women with PCOS continues to evolve, underscoring the significance of developing more comprehensive strategies for women's reproductive health, particularly during significant life stages like perimenopause and menopause.
Conclusion
GLP-1 receptor agonists have emerged as a groundbreaking class of medications for managing type 2 diabetes and associated metabolic disorders. By simulating natural hormones, these medications enhance appetite regulation, improve insulin sensitivity, and support sustainable weight loss. This nuanced understanding of GLP-1 therapy's synergy with physical activity and nutrition can empower healthcare providers and patients to collectively tackle the complexities of insulin-related disorders and improve overall well-being.